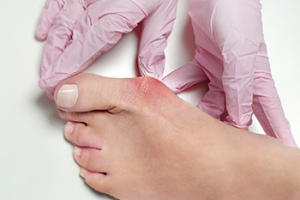
Common Symptoms of Bunions

Bunions, a prevalent foot deformity, reveal themselves through an array of recognizable symptoms. One telltale sign is the development of a bony bump at the base of the big toe, often accompanied by redness and swelling. As the tip of the big toe deviates toward the adjacent toes, persistent pain or soreness ensues, particularly when walking or wearing shoes. Corns or calluses may form where the first and second toes overlap, exacerbating discomfort. Limited toe movement and stiffness can impede flexibility. Shoes that once fit comfortably may now cause tightness and discomfort, reflecting the altered shape of the foot. Recognizing these common symptoms is pivotal for timely intervention. By understanding these subtle yet critical signs, individuals can take proactive steps towards managing bunions and nurturing overall foot health. If you have developed a bunion, it is strongly suggested that you are under the care of a podiatrist who can determine what the best relief and treatment is for you.
If you are suffering from bunion pain, contact Kent DiNucci, DPM of Ankle and Foot Clinic . Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is a Bunion?
Bunions are painful bony bumps that usually develop on the inside of the foot at the joint of the big toe. As the deformity increases over time, it may become painful to walk and wear shoes. Women are more likely to exacerbate existing bunions since they often wear tight, narrow shoes that shift their toes together. Bunion pain can be relieved by wearing wider shoes with enough room for the toes.
Causes
- Genetics – some people inherit feet that are more prone to bunion development
- Inflammatory Conditions - rheumatoid arthritis and polio may cause bunion development
Symptoms
- Redness and inflammation
- Pain and tenderness
- Callus or corns on the bump
- Restricted motion in the big toe
In order to diagnose your bunion, your podiatrist may ask about your medical history, symptoms, and general health. Your doctor might also order an x-ray to take a closer look at your feet. Nonsurgical treatment options include orthotics, padding, icing, changes in footwear, and medication. If nonsurgical treatments don’t alleviate your bunion pain, surgery may be necessary.
If you have any questions, please feel free to contact our office located in Omaha, NE . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Bunions
A bunion is a bump that forms at the base of the big toe. Bunions form when the big toe pushes against the next toe, which forces the big toe joint to get bigger and stick out. As a result, the skin over the bunion may start to appear red and it may feel sore.
There are risk factors that can increase your chances of developing bunions. People who wear high heels or ill-fitting shoes are more likely to develop them, in addition to those who have a genetic history of bunions or have rheumatoid arthritis.
The most obvious way to tell if you have a bunion is to look for the big toe pushing up against the toe next to it. Bunions produce a large protrusion at the base of the big toe and may or may not cause pain. Other symptoms are redness, swelling, and restricted movement of the big toe if you have arthritis.
Nonsurgical methods are frequently used to treat bunions that aren’t severe. Some methods of nonsurgical treatment are orthotics, icing and resting the foot, taping the foot, and pain medication. Surgery is usually only required in extreme cases. However, if surgery is needed, some procedures may involve removing the swollen tissue from around the big toe joint, straightening the big toe by removing part of the bone, or joining the bones of your affected joint permanently.
Your podiatrist will diagnose your bunion by doing a thorough examination of your foot. He or she may also conduct an x-ray to determine the cause of the bunion and its severity.
Causes of Foot Stress Fractures

A foot stress fracture, a condition prevalent among athletes and individuals engaged in repetitive weight-bearing activities, is characterized by tiny cracks in the bones of the foot. These fractures often result from overuse, with excessive and repetitive impact on the feet causing structural fatigue. Contributing causes include sudden increases in physical activity, improper footwear, or inadequate training surfaces. Symptoms manifest gradually, beginning with localized pain during activity that subsides with rest. As the stress fracture progresses, the pain becomes persistent, and swelling may occur. Tenderness to touch, particularly at specific points on the foot, is a common indicator. Ignoring these symptoms can lead to more severe fractures, potentially requiring prolonged recovery. Understanding the definition, causes, and symptoms of foot stress fractures is essential for individuals engaged in high-impact activities. If you have a foot stress fracture, it is suggested that you make an appointment with a podiatrist who can guide you toward the best treatment.
Stress fractures occur when there is a tiny crack within a bone. To learn more, contact Kent DiNucci, DPM from Ankle and Foot Clinic . Our doctor can provide the care you need to keep you pain free and on your feet.
How Are They Caused?
Stress fractures are the result of repetitive force being placed on the bone. Since the lower leg and feet often carry most of the body’s weight, stress fractures are likely to occur in these areas. If you rush into a new exercise, you are more likely to develop a stress fracture since you are starting too much, too soon. Pain resulting from stress fractures may go unnoticed at first, however it may start to worsen over time.
Risk Factors
- Gender – They are more commonly found in women compared to men.
- Foot Problems – People with unusual arches in their feet are more likely to develop stress fractures.
- Certain Sports – Dancers, gymnasts, tennis players, runners, and basketball players are more likely to develop stress fractures.
- Lack of Nutrients – A lack of vitamin D and calcium may weaken the bones and make you more prone to stress fractures
- Weak Bones – Osteoporosis can weaken the bones therefore resulting in stress fractures
Stress fractures do not always heal properly, so it is important that you seek help from a podiatrist if you suspect you may have one. Ignoring your stress fracture may cause it to worsen, and you may develop chronic pain as well as additional fractures.
If you have any questions, please feel free to contact our office located in Omaha, NE . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Stress Fractures of the Foot and Ankle
Our bones are important aspects of our body and they are constantly changing. The heavier the workload for a bone, the more likely it is that calcium will be placed in it. When a bone isn’t used often, there won’t be much calcium within it. When stress from repetitive loads prevent the bone from being able to repair itself, cracks will start to form. Stress fractures are defined as cracks in a bone that result from repetitive force, such as overuse.
The most common cause of stress fractures is a sudden increase in intensity and duration of physical activity. For example, if you begin to run long distances without working your way into doing so, you will be more likely to develop a stress fracture.
Common symptoms of stress fractures are pain and swelling near the weight bearing area on the injured bone. When initial x-rays are performed, it is possible that the fracture will not show up. However, once the stress on the area continues, the damage will increase, and the fracture will be severe enough to show up on an x-ray. Certain parts of the foot are more likely to develop stress fractures than others. Areas that typically have these fractures are: the metatarsals, the navicular bone, the calcaneus, tibia, and fibula.
Since women are at an increased risk of developing osteoporosis, they are twice as likely as men to sustain a stress fracture. Additionally, old age causes a decrease in bone mineral density which is why elderly people are also likely to develop these fractures.
It is important for you to be professionally diagnosed by a podiatrist if you suspect you have a stress fracture, because there are other injuries that can easily be mistaken for a fracture. Sprains, strains, shin splints, plantar fasciitis, and Morton’s neuroma can all easily be mistaken for stress fractures in the foot. Your podiatrist will likely ask you a series of questions to determine what type of pain you are experiencing. These questions will help your doctor identify whether you have a stress fracture.
The best method of treatment for a stress fracture is rest. Additionally, a walking boot, cast, or crutches, will help rest the area that is injured. The typical healing time for stress fractures is 4-12 weeks, however this depends on which bone is involved.
Occupational Hazards of Plantar Fasciitis

Plantar fasciitis is prevalent in manufacturing environments, with several factors influencing its occurrence. These can include forefoot pronation during physical examination, high metatarsal pressure in gait assessments, and prolonged standing on hard surfaces. The rotation of footwear during the workweek appears to reduce the likelihood of developing plantar fasciitis. Using shoe orthoses with medial longitudinal arch and metatarsal pads can serve as a preventive or treatment approach. Implementing workstations that reduce the time spent walking or standing on hard surfaces, such as offering cushioning mats or alternating sitting and standing postures, may help lower the risk of plantar fasciitis. If you work in manufacturing and have developed heel pain, it is suggested that you schedule an appointment with a podiatrist for a proper diagnosis, treatment, and additional preventative advice.
Plantar fasciitis can be very painful and inconvenient. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Kent DiNucci, DPM from Ankle and Foot Clinic . Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is the inflammation of the thick band of tissue that runs along the bottom of your foot, known as the plantar fascia, and causes mild to severe heel pain.
What Causes Plantar Fasciitis?
- Excessive running
- Non-supportive shoes
- Overpronation
- Repeated stretching and tearing of the plantar fascia
How Can It Be Treated?
- Conservative measures – anti-inflammatories, ice packs, stretching exercises, physical therapy, orthotic devices
- Shockwave therapy – sound waves are sent to the affected area to facilitate healing and are usually used for chronic cases of plantar fasciitis
- Surgery – usually only used as a last resort when all else fails. The plantar fascia can be surgically detached from the heel
While very treatable, plantar fasciitis is definitely not something that should be ignored. Especially in severe cases, speaking to your doctor right away is highly recommended to avoid complications and severe heel pain. Your podiatrist can work with you to provide the appropriate treatment options tailored to your condition.
If you have any questions please feel free to contact our office located in Omaha, NE . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Plantar Fasciitis
The plantar fascia is a connective tissue in the heel that stretches across the bottom length of your foot. Plantar fasciitis occurs when the connective tissue becomes inflamed, causing heel pain and discomfort during physical activity. Although the condition is completely treatable, traditional methods can take up to a year to start becoming effective.
Plantar fasciitis is caused by a number of everyday activities, so understanding the condition is important for managing and treating it. One of the most common causes of plantar fasciitis is excessive running, especially with improper fitting or non-supportive shoes. Too much exercise can lead to the plantar fascia being overworked and overstretched, which can cause tears in the tissue. Along with improper fitting shoes, pronation, the rolling of the feet inward, is a common cause of plantar fasciitis. If not treated properly, the plantar fascia becomes overstretched and starts to tear, causing inflammation.
Despite the common causes of plantar fasciitis, there are many different treatment options. For less severe cases, conservative home remedies include taking anti-inflammatory drugs to alleviate pain, applying ice packs to the bottom of your foot and heel, slowly stretching and exercising your feet to re-strengthen the tissue, and using orthotic devices are all ways to help manage your plantar fasciitis.
For more severe cases, shockwave therapy has become a common solution for plantar fasciitis. Shockwave therapy can effectively break up the tissue on the bottom of your foot which facilitates healing and regeneration. This fights the chronic pain caused by plantar fasciitis. Even if this doesn’t work, surgery is always a final option. Surgery on the tissue itself can be done to permanently correct the issue and stop the inflammation and pain in your heels.
No matter what the case may be, consulting your podiatrist is the first and best step to recovery. Even the slightest amount of heel pain could be the first stage of plantar fasciitis. Untreated symptoms can lead to the tearing and overstretching of tissue. Because the tearing of tissue can be compounded if it remains ignored, it can evolve into a severe case. The solution is early detection and early treatment. Talk to your podiatrist about the possibilities of plantar fasciitis if you’re experiencing heel pain.
How to Select the Ideal Running Shoe

Choosing the right running shoe is a critical decision that directly impacts both comfort and performance. Different foot types and running styles necessitate a personalized approach to ensure the perfect fit. For those individuals with high arches, cushioned shoes with ample shock absorption help absorb impact and provide essential support. Conversely, individuals with low arches or flat feet benefit from stability shoes that offer extra arch support and motion control. Runners who overpronate or supinate require shoes designed to address their specific gait patterns, preventing potential injuries. Determining your foot type and understanding your running mechanics are pivotal in guiding the selection process. Ultimately, investing time in finding the right running shoe tailored to your individual needs enhances not only the running experience but also safeguards against potential discomfort and injury. If you would like specific information about how to find the right running shoes for your needs, it is suggested that you consult a podiatrist.
If you are a runner, wearing the right running shoe is essential. For more information, contact Kent DiNucci, DPM from Ankle and Foot Clinic . Our doctor can provide the care you need to keep you pain-free and on your feet.
Choosing the Right Running Shoe for Your Foot Type
To increase performance and avoid the risk of injury, it is important to choose the right running shoe based on your foot type. The general design of running shoes revolves around pronation, which is how the ankle rolls from outside to inside when the foot strikes the ground.
- Neutral runners are able to choose from a wide variety of shoes, including minimalist shoes or even going barefoot.
- Runners who overpronate, or experience an over-abundance of ankle rolling, should choose shoes that provide extra motion control and stability.
- Runners who underpronate, or supinate, have feet that have high arches and lack flexibility, preventing shock absorption. They require shoes with more flexibility and cushion.
If you have any questions please feel free to contact our office located in Omaha, NE . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Choosing the Right Running Shoe
Choosing the right running shoes for you is an important part of running. A good pair of running shoes will make the running experience more enjoyable for you and prevent potential injury.
Poorly-fitted shoes can increase the risk of injury in runners substantially. Common injuries from running with poor quality shoes include shin splints, sprained ankles, Achilles tendinitis, stress fractures, plantar fasciitis and more. This is due to the fact that bad shoes do not provide proper foot support, can increase pronation (how much the foot rolls when hitting the ground), have little to no cushioning, do not allow the feet to breath, and do not provide enough flex and rigidity in the right parts.
When looking for running shoes, first, determine where you will be running. If you are a trail runner, then pick trail shoes. If you run on concrete and asphalt, then regular running shoes are the best choice. When trying on shoes, its best to go at the end of the day as feet grow during the day and shrink after a night of sleep. Shoes should be more rigid towards the back of the foot while being more flexible up where the toes are. The toe box should provide enough room for the toes to move freely. The overall fit should be snug, not too tight but not too loose. A good pair of running shoes should also provide enough arch support for your foot type. If you experience overpronation or under-pronation while running, try to find a pair of shoes that will help correct this with different sole patterns. Finally, try to find a pair of shoes that allow the feet to breathe like nylon mesh or synthetic leather.
Don’t forget about the socks either. Socks that hold too much moisture can lead to athlete’s foot. Socks should be breathable so that your feet can air out and breathe. Synthetic socks wick away moisture like sweat. If you tend to run a lot, having a second pair of shoes that you can wear while you let the first pair air out is smart. Just don’t forget to replace your shoes after about every 300 to 500 miles.
Before you start running, it is advised to see a podiatrist to see if running is right for you. They can also offer good advice on how to run and what to look for in a pair of running shoes. If you have flat feet or poorly supported ones, they can also offer custom-made orthotics that will help give your feet the support they need.
Mobility and Balance Problems in the Elderly

As people age, they often encounter mobility challenges, impacting their ability to move freely. These issues encompass unsteadiness while walking, difficulty in sitting or standing, and the risk of falling. Various factors contribute to these mobility problems in older individuals, including muscle weakness, joint ailments, pain, underlying diseases, and neurological difficulties. Sometimes, multiple mild issues combine, severely affecting mobility. The most common mobility concern among seniors is the risk of falling, which can lead to fractures, injuries, and a persistent fear of falling. Older bones are more fragile and take longer to heal. In cases of minor falls without serious injuries, assisting the person in getting up is vital. If the individual is in pain or injured, it is best to summon help. However, if they can move, they should crawl to a stable chair and use it for support. Falls can result in reduced mobility or bed rest, exacerbating existing medical conditions and leading to new health issues. Encouraging physical activity is essential to combat the fear of falling and its associated inactivity. Even minimal exercise strengthens bones and muscles, enhancing steadiness and preventing fractures. Additionally, conducting a home safety assessment and addressing potential hazards can further prevent falls. If you are a senior or caring for one, it is suggested that you schedule an appointment with a podiatrist for a thorough consultation and communication of any mobility problems and falls.
Proper foot care is something many older adults forget to consider. If you have any concerns about your feet and ankles, contact Kent DiNucci, DPM from Ankle and Foot Clinic . Our doctor can provide the care you need to keep you pain-free and on your feet.
The Elderly and Their Feet
As we age we start to notice many changes in our body, but the elder population may not notice them right away. Medical conditions may prevent the elderly to take notice of their foot health right away. Poor vision is a lead contributor to not taking action for the elderly.
Common Conditions
- Neuropathy – can reduce feeling in the feet and can hide many life-threatening medical conditions.
- Reduced flexibility – prevents the ability of proper toenail trimming, and foot cleaning. If left untreated, it may lead to further medical issues.
- Foot sores – amongst the older population can be serious before they are discovered. Some of the problematic conditions they may face are:
- Gouging toenails affecting nearby toe
- Shoes that don’t fit properly
- Pressure sores
- Loss of circulation in legs & feet
- Edema & swelling of feet and ankles
Susceptible Infections
Diabetes and poor circulation can cause general loss of sensitivity over the years, turning a simple cut into a serious issue.
If you have any questions please feel free to contact our office located in Omaha, NE . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Elderly Foot Care
As you grow older, you will start to notice more problems with your feet due to wear and tear. This may also happen because the skin will start to become thin and lose elasticity. Some signs of aging feet are regular aches and pains, bunion development, and clawed toes.
Fortunately, there are ways you can improve comfort, relieve pain, and maintain mobility in your feet. One of the best ways to deal with aging feet is to exercise. If you keep active, your muscles will become toned which will then strengthen the arches in the foot and stimulate blood circulation.
It is important that you practice proper foot care to protect your aging feet. You should wash your feet in warm water on an everyday basis. Afterward, the feet need to be dried well and it is important to dry between the toes. Your toenails should be trimmed and kept under control; nails that are poorly cut may become ingrown. At the end of each day, performing an inspection of your feet will allow you to detect any ailments in their early stages.
As you grow older, it becomes more important that you wear comfortable shoes. Your shoes should be secure, and they should provide decent arch support. If you are looking to buy a new pair of shoes, it is best to look for a pair that are made from a breathable material. It is also helpful to have shoes that have a bit of extra room at the top of the shoe, especially if you suffer from swollen feet.
The most common foot problems that elderly people will encounter are bunions, calluses, corns, hammertoes, heel pain, and foot problems related to diabetes. Some other issues include arch pain, tarsal tunnel syndrome, Achilles tendonitis, and Morton’s neuroma
An annual foot examination is a great way for you to ensure that you do not have any serious health problems with your feet. You should talk to a podiatrist about the available treatment options for whichever foot issue you are dealing with.